The Truth About the “Alzheimer’s Gene”

Alzheimer’s disease is a devastating condition that affects millions of individuals worldwide, robbing them of their memories and cognitive abilities. In recent years, there has been much discussion about a specific gene, APOE4, often referred to as the “Alzheimer’s gene.” There is a lot of misconception that having the APOE4 gene guarantees the development of […]
Do You Know the Top 9 Food Allergens?

Almost 90% of all serious food allergies are caused by just a few foods. These foods are often ingredients in other foods, so avoiding them requires diligence, including careful label reading and other measures. Even then, there may be times when exposures happen unknowingly. This blog covers some of the foods and products you’ll need […]
Do I Need A Multivitamin?

Do I need a multivitamin? This is a common question I am asked. I think most of us should be taking a high quality multivitamin these days, even if we’re eating a healthy diet. It is difficult to meet nutrient needs from food alone because of the following five reasons. Declining soil quality Increasing toxic […]
The 5 Best (and Worst) Sweeteners You Can Eat

Let’s face it: Sweeteners aren’t great for your health. They stimulate your appetite, encourage your sweet tooth and pack on the pounds while also placing you at risk for obesity, type 2 diabetes, heart disease and fatty liver. But, we’re all human and cutting all sweeteners tomorrow isn’t realistic. Let’s rank the best and worst […]
Want to Screen for Diabetes Risk?
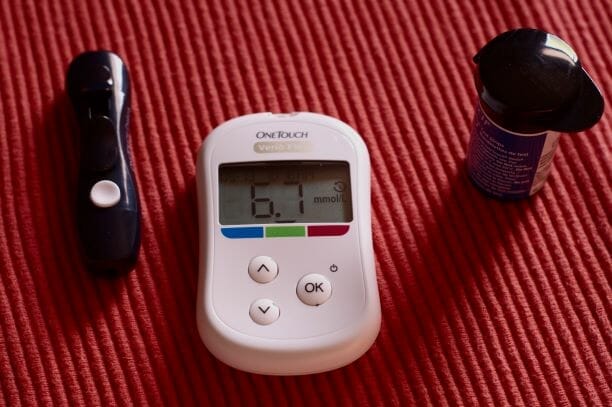
Want to screen for diabetes risk? With so many people living with diabetes, the term is used so often that we either think that we will never get this, or that if we do there are many medications that will keep it under control. But what we can’t picture are all the risks – blindness, […]
Depressed? Check Your Gut Bacteria

Depressed? Check Your Gut Bacteria The Wall Street Journal has an article on this on December 22, 2020. Yes! At last, the realization that depression is a condition of inflammation (not a chemical imbalance of the brain) is gaining widespread attention. “The field of psychiatry has known about the role of the immune system in […]
A New Vaccine – Optimize Your Brain PODCAST
In my latest PODCAST I talk about a new book I am so excited about. The End of Alzheimer’s Program, Dr Dale Bredesen , MD talks about needing a new vaccine for Alzheimer’s Disease. Not an injection, but a personalized lifestyle program based on all the contributing factors. He lays out the detailed program he […]
Key Biomarkers for Alzheimer’s disease
Did you know there are key biomarkers for Alzheimer’s disease? Whether a person is at risk of developing the disease versus actively has symptoms, is often reflective of the number of their biomarkers. As few as three to five suboptimal lab values may be observed in an at-risk pre-symptomatic person versus up to 25 in […]
WHAT IS NUTRIGENOMICS? – Podcast

Have you heard about Nutrigenomics? In this episode of Dr Karen Health Talks, I explain how we are not victims of our genes. In fact with the human genome project showing that humans have the same number of genes as worms, there is a whole new understanding of the cause of human variation. I use […]





















